There are benefits to having a baby after 35 years old. Older women and birthing people are more likely to show an increase in happiness after having a baby than those younger than them (Myrskylä et al, 2017).
Our NCT Antenatal classes provide up-to-date, evidence-based information to help make decisions about your parenting journey.
Likelihood of getting pregnant after having sex
No matter what your age, the biggest factor in getting pregnant is how often you have sex (BPAS, No date). The more you have sex, the more likely you are to get pregnant.
There is a slight increase in difficulty becoming pregnant as you get older (NICE, 2013).
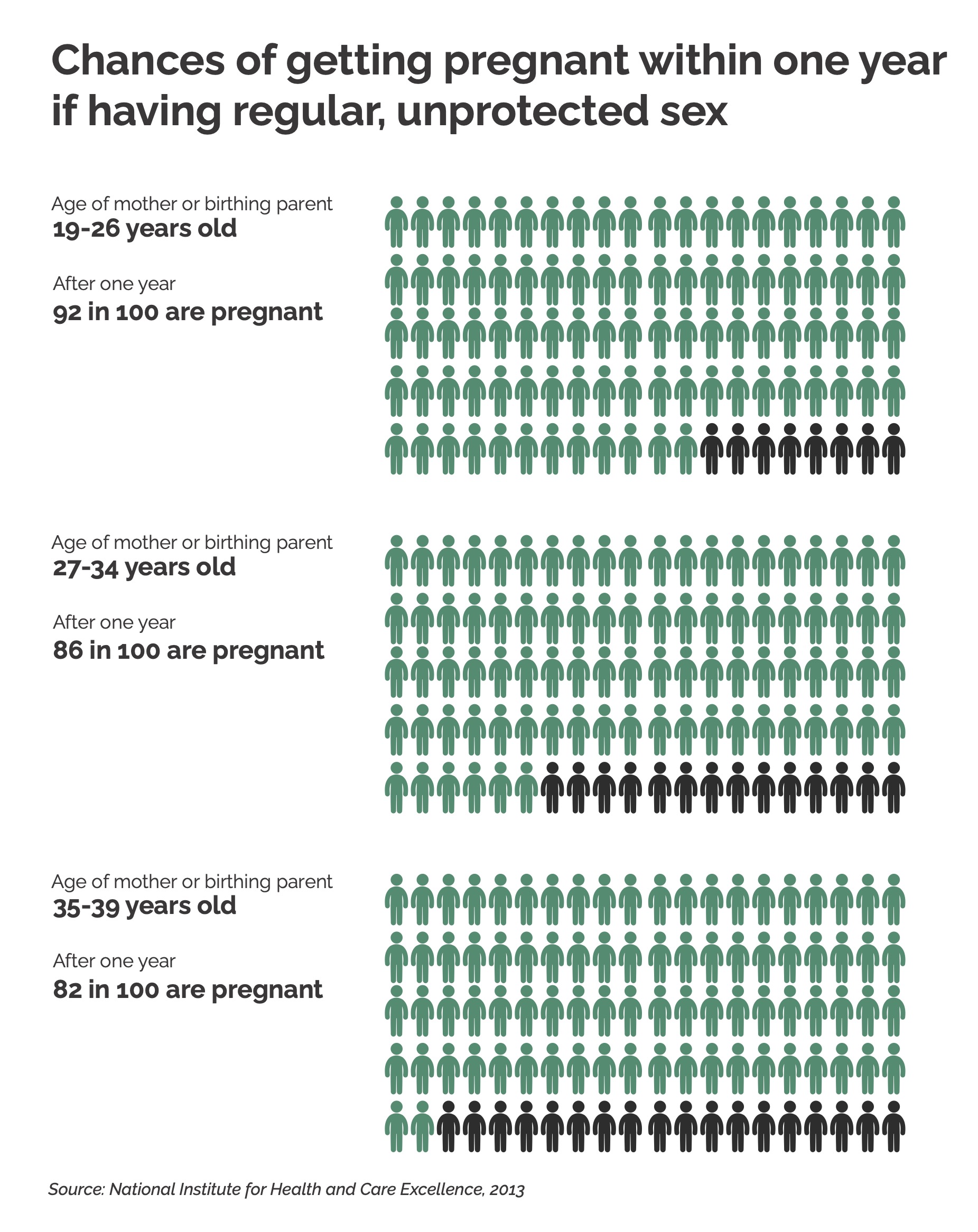
If you have trouble getting pregnant over the course of a year, it is likely you will get pregnant if you carry on trying for another year (NICE, 2013).
After the age of 35, the age of the father is as much a factor as the woman’s age (NICE, 2013).
Likelihood of getting pregnant by artificial insemination
For those not having sex to get pregnant, the pattern of fertility reducing with age is the same, but with a lower starting point.
- For those under 35, between 50 and 60 in 100 are pregnant after one cycle (or one year of IUI), and between 40 and 50 in 100 are not.
- For those over 35, between 33 and 50 in 100 are pregnant after one cycle (or one year of IUI), and between 50 and 67 in 100 are not.
The chances of being pregnant increases with more cycles.
Risks of having a baby after 35
The birth of a first baby is more likely to be complicated than having a subsequent baby, no matter how old you are.
As people get older, the chance of other health issues rises. These health issues are what is relevant, and not the age by itself (Morris et al, 2018).
Conditions associated with higher maternal age include (Fuchs et al, 2018):
- Chronic hypertension
- Gestational diabetes
- Placenta praevia
Hypertension of pregnancy is more likely in parents under 30, less likely between 30 and 34, and then more likely over 35 (Fuchs et al, 2018).
Other factors to consider
Older women and birthing people are also more likely to (Fuchs et al, 2018):
- Use assisted reproduction techniques, such as in vitro fertilisation (IVF)
- Have invasive procedures in pregnancy, like amniocentesis.
The chance of having a baby with a fetal anomaly such as Down, Edwards or Patau’s syndromes increases from the age of 25. It is highest over the age of 45. Older women and birthing people are also more likely to have multiple pregnancies (such as twins or triplets) (BPAS, No date).
Is my baby more likely to be born early?
Some research suggests that premature birth (babies born before 37 weeks) follows a U-shaped curve. This would mean that most cases are found in those under the age of 25 or over the age of 40 (Fuchs et al, 2018).
This research found that premature birth happened naturally to women and birthing people under 25. For those over 40 it followed induction or caesarean birth (Fuchs et al, 2018).
Other research removed potential reasons for premature birth such as social background or genetic factors. This then found that maternal age had no effect on the chance of premature birth (Goisis et al, 2017).
Is miscarriage more likely over 35?
The chance of miscarriage increases to older mothers and fathers, and is most likely if the mother is over 35 and the father is over 40. But you are still more likely to have a healthy pregnancy than a miscarriage even if you are over 40 (Miscarriage, why me?).
Implications for care for those over 35
Antenatal care and care in labour
Antenatal care and care in labour for women and birthing people over the age of 35 is the same as for those under 35 unless there are other risk factors (NICE, 2021a; NICE, 2023).
Pre-eclampsia and gestational hypertension
Pre-eclampsia and gestational hypertension are moderate risk factors for women and birthing people over 40. This will lead to them being offered additional antenatal care (NICE, 2019).
Induction and caesarean birth
Doctors may offer induction earlier (at 40 weeks rather than 41-42 weeks) to reduce any possible impact on the baby (Knight et al, 2017). However, this is not included in the NICE guideline for induction of labour (NICE, 2021b).
Following a caesarean birth, the mother or birthing person has a higher risk of serious complications if they are over 35 years old (Korb et al, 2019).
How to stay healthy
As with any pregnancy it is important to eat healthily and exercise regularly. It’s also important to access antenatal care.
Smoking was found to be a greater risk of death for mothers or birthing people over 35 than for younger parents (McCall et al, 2017). You can access NHS services to help you quit.
Advantages of being an older parent
Research suggests that older parents may be more likely to look after themselves while pregnant. For example, by drinking less alcohol and seeing the value in antenatal care. This might help offset any negative effects of being pregnant at an older age (Goisis et al, 2017).
Older parents tend to have gained education and social stability, which might explain why they have been found to be happier than younger parents (Myrskyla et al, 2017).
Further information
Our in-person NCT Antenatal courses give you up-to-date, evidence-based information to help you make decisions about your birth, your baby, your options.
Find out more about life after you've given birth on our NCT New Baby course. It supports new parents and their babies, leaving you feeling confident, knowledgeable and relaxed.
BPAS (No date) “Older” motherhood. https://www.bpas.org/our-cause/campaigns/briefings/older-motherhood/ [30 Sep 24]
Fuchs F, Monet B, Ducruet T, Chaillet N, Audibert F (2018) Effect of maternal age on the risk of preterm birth: A large cohort study. PLoS ONE 13(1): e0191002. https://doi.org/10.1371/journal.pone.0191002
Goisis A, Remes H, Barclay K, Martikainen P, Myrskylä M. (2017) Advanced Maternal Age and the Risk of Low Birth Weight and Preterm Delivery: a Within-Family Analysis Using Finnish Population Registers. Am J Epidemiol. Dec 1;186(11):1219-1226. https://doi.org/10.1093/aje/kwx177
Knight HE, Cromwell DA, Gurol-Urganci I, Harron K, van der Meulen JH, Smith GCS (2017) Perinatal mortality associated with induction of labour versus expectant management in nulliparous women aged 35 years or over: An English national cohort study. PLoS Med 14(11): e1002425. https://doi.org/10.1371/journal.pmed.1002425
Korb D, Goffinet F, Seco A, Chevret S, Deneux-Tharaux C, From EPIMOMS Study Group. (2019) Risk of severe maternal morbidity associated with caesarean delivery and the importance of maternal age: A population-based propensity score analysis. European Journal of Obstetrics & Gynecology and Reproductive Biology, 234, e113. https://doi.org/10.1016/j.ejogrb.2018.08.407
McCall, SJ, Nair, M, Knight, M. (2017) Factors associated with maternal mortality at advanced maternal age: a population-based case–control study. BJOG: An International Journal of Obstetrics & Gynaecology. 124 (8) 1470-0328. https://doi.org/10.1111/1471-0528.14216
Miscarriage Association (2024) Why me? Available from: https://www.miscarriageassociation.org.uk/information/miscarriage/ [Accessed 28 Feb 24]
Morris JM, Totterdell J, Bin YS, Ford JB, Roberts CL. (2018) Contribution of maternal age, medical and obstetric history to maternal and perinatal morbidity/mortality for women aged 35 or older. Aust N Z J Obstet Gynaecol. Feb;58(1):91-97. https://doi.org/10.1111/ajo.12674
Myrskylä M, Barclay K, Goisis A. (2017) Advantages of later motherhood. Gynakologe. 50(10):767-772. https://doi.org/10.1007/s00129-017-4124-1
NICE (2013) Fertility problems, assessment and treatment [CG156]. https://www.nice.org.uk/guidance/cg156 [21 Oct 24]
NICE (2019) Hypertension in pregnancy [NG133]. http://www.nice.org.uk/guidance/ng133 [30 Sep 24]
NICE (2021a) Antenatal care [NG201] https://www.nice.org.uk/guidance/ng201 [11 Oct 24]
NICE (2021b) Inducing labour [NG207]. https://www.nice.org.uk/guidance/ng207 [30 Sep 24]
NICE (2023) Intrapartum care [NG235]. https://www.nice.org.uk/guidance/ng235 [31 Oct 24]