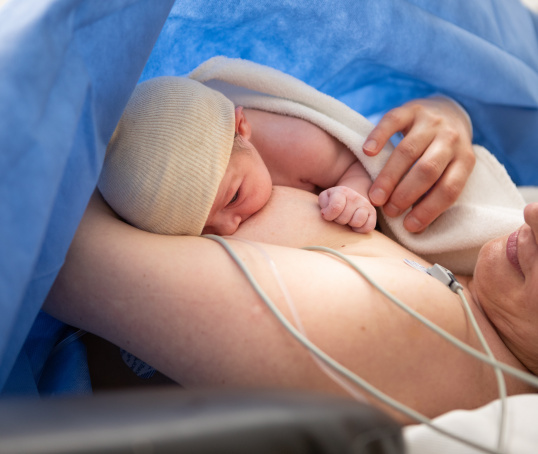
For information on attachment and positions, read our article on breastfeeding positions.
Why breastfeed?
Many people intend to breastfeed. This is because the milk:
- contains all the nutrients and hormones a baby needs to grow and develop, and is easy to digest (NHS, 2022)
- is a living product, which changes from feed to feed to meet the baby’s needs for growth, development and protection (La Leche League GB, 2021; Riskin et al, 2012)
- is rich in the immune-protecting ingredients which reduce infections and support development (Kim & Yi, 2020; NHS, 2022)
- contains the microbes which boost the baby’s microbiome and gut immunity (Kim & Yi, 2020; NHS, 2022)
- is especially beneficial for protecting premature or poorly babies from infection (NHS, 2023a)
And because there is no manufacturing process or packaging, breastmilk has no negative impact on the environment.
Are there any drawbacks?
Breastfeeding is a learnt skill for both parent and baby, and it can take a while to work out how to do it. But when you and your baby have the hang of it, it can be easy to do whenever and wherever you are.
Breastfeeding does take time. And if the breastfeeding parent expresses milk so that someone else can feed the baby, that also takes time.
Can everyone breastfeed?
A small number of women and birthing people will be advised not to breastfeed for a medical reason. This might be because of an infection or medication being taken for another condition (NHS, 2023a).
A few have a medical condition such as polycystic ovary syndrome, or breast hypoplasia, which means they might not make enough milk to breastfeed exclusively (Breastfeeding Network, no date).
Breastfeeding after breast surgery
Women who have had breast implants should be able to breastfeed, but it will depend on the type of incision (NHS Start for Life, no date). The NHS has more information.
Some women who have had breast reduction may not be able to breastfeed, depending on the type of surgery (NHS, 2023d). This is something to discuss with the doctor.
What are the different kinds of breastmilk?
Colostrum
The first milk the breasts produce is called colostrum. It is produced from the second trimester of pregnancy. This concentrated milk is thick and often a golden yellow colour.
It’s concentrated as the baby can only take very small feeds of about a teaspoonful in the early days. So the baby will feed very frequently, perhaps hourly (NHS, 2023b).
The baby is learning to breastfeed, so a feed may feel like it takes a long time for a small amount of fluid. But this practice helps to establish the mother or feeding parent's milk supply as well as developing the baby's feeding techniques and stamina.
Colostrum provides the baby with (La Leche League GB, 2021; Kim & Yi, 2020):
- carbohydrates
- protein
- fat
- vitamins and minerals
- antibodies
- hormones and growth factors
Mature milk
Two to four days after birth, breasts might feel fuller as the volume of milk increases. At first this can feel uncomfortable, and can result in engorgement. Continuing to offer the baby frequent feeds can help to ease engorgement (La Leche League GB, 2021; NHS, 2023b).
As the milk matures, feeds get longer and a little less frequent (NHS, 2023b).
Mature milk is essentially colostrum diluted with water. It looks thinner than colostrum and can be a blue-white colour. It contains the same nutrients, hormones and growth factors that help the baby develop (Kim & Yi, 2020; La Leche League GB, 2021).
However, colostrum is lower in fat, and mature milk is higher. This is because in the very early days the newborn needs more carbohydrate than fat (Kim & Yi, 2020).
How does milk meet the babies’ needs?
During each feed the fat content gradually increases. So every feed starts out as lower fat and more thirst quenching. As the feed goes on it becomes higher fat (La Leche League GB, 2021).
Babies end a feed when they have had enough calories. Allowing the healthy baby to remain on the breast until they are ready to come off means they meet their own nutritional needs. It is not possible to overfeed a breastfed baby (Kim & Yi, 2020; La Leche League GB, 2021; NHS, 2023b).
How do the breasts make the right amount of milk?
The size of the breasts doesn’t affect how much milk is made (La Leche League GB, 2021).
In the first few weeks, babies feed often, at least 8 times in 24 hours, although 10-12 or more times is ideal (La Leche League GB, 2021; NHS, 2023a). This:
- is when the baby is hungry or needs comfort, and not necessarily evenly spaced throughout the day
- needs to include night feeds (NHS, 2023b)
- stimulates milk production – as the breast empties, more milk is made (NHS, 2023b)
Expressing is another way of stimulating milk production if the baby isn’t feeding directly from the breast (La Leche League GB, 2021).
Over time the number of feeds in 24hrs will reduce as the baby gets more efficient at feeding (La Leche League GB, 2021).
The mother or feeding parent and baby’s bodies work together to make the amount of milk the baby needs. It’s impossible to fully ‘empty’ the breasts. As milk is taken out, the body signals to replace it (La Leche League GB, 2021).
This is how it’s possible to feed twins or more. And why not emptying the breasts leads to reduced or stopped milk production within a couple of weeks (La Leche League GB, 2021; NHS, 2023a).
How will I know how to breastfeed?
Breastfeeding is a skill that the mother or feeding parent and baby or babies learn together in the early days. This can take some time as they get to know each other (NHS, 2023a). Our article on attachment and positioning might help get started.
Every feeding journey is unique, so even if breastfeeding goes well with one baby, it might take some time to get the hang of it with another baby (La Leche League GB, 2021).
Our Breastfeeding Counsellors are on hand every day of the year, from 8am to midnight, to answer any questions about all types of feeding. Call 0300 330 0700.
What can increase the chances of successfully breastfeeding?
Before birth
It can help to be prepared and know what to expect (NHS, 2023b). Our NCT Antenatal class has a dedicated session about feeding, where you’ll learn about positions, attachment, how to get support and more.
Immediately after birth
Putting the baby onto the mother or birthing parent’s bare chest is called skin-to-skin contact. It can (NHS, 2023b):
- keep the baby warm
- calm them and steady their breathing
- support natural breastfeeding behaviours
- encourage the baby to attach to the breast using a natural crawling and latching-on reflex
If there is a delay such as the baby going to special care, skin-to-skin contact can be done when possible (NHS, 2023b).
Skin-to-skin at any time as the baby gets older can support effective breastfeeding.
What is the let-down reflex?
The let-down reflex (often referred to as ‘let-down’) is when muscles in the breast squeeze milk to the nipples. Some people experience a strong tingling feeling in the early weeks, and others don’t feel anything (NHS, 2023b).
This response happens when the baby is sucking on the breast, and sometimes when hearing a baby crying (NHS, 2023b).
When milk begins to flow, the baby’s sucking pattern changes to slower, deeper sucks, along with swallowing that you might be able to see or hear (NHS, 2023b).
If the baby coughs or splutters when the milk begins to flow after let-down, changing to a more laid-back position might help.
If the baby falls asleep before milk has been released, they may not be getting enough milk. A midwife, health visitor or Breastfeeding Counsellor should be able to help with any concerns about breastfeeding (NHS, 2023b).
You can call our Breastfeeding Counsellors every day of the year from 8am to midnight on 0300 330 0700 with any questions or worries about feeding.
How long to feed?
How long is each feed?
A rough guide is that the baby is feeding at least 8 and ideally 10-12 or more times in 24 hours. However, these feeds will not be evenly spaced or all the same volume. Just like adults, babies sometimes want a snack or a drink, and sometimes a full meal. This means some feeds will be short, and others long (NHS, 2023a).
It’s recommended to let the baby finish a feed at one breast, then offer the other. If they’ve had enough, they won’t take any more (NHS, 2023a).
What is responsive feeding?
Breastfeeding is about food, comfort and reassurance. Responsive feeding, where a feed is offered whenever they show feeding cues, is allowing the baby to lead the feeding process (NHS, 2023a).
In the very early days feeds may be very frequent. As they get older, feeds will tend to spread out. If they’re unwell or going through a growth spurt, they may want lots of cuddles and feeds (NHS, 2023a).
It’s also about responding to your own needs. If the breasts are uncomfortably full, if it’s necessary to feed before going out, or you’d just like a cuddle with your baby, you can offer a feed (NHS, 2023a).
How long is a breastfeeding relationship?
It is recommended to exclusively breastfeed for the first six months. This means offering nothing but breastmilk (NHS, 2023a).
Breastmilk can then be offered alongside introducing solids from six months. It continues to be an excellent nutrition for as long as both parent and baby feel comfortable feeding (NHS, 2023a). The World Health Organisation (WHO) and UNICEF (United Nations Children’s Fund) recommend breastfeeding up to two years and beyond (WHO, no date).
Positions and attachment
Effectively attaching the baby to the breast and finding a comfortable position to feed in are important for successful breastfeeding. Our article on breastfeeding positions explains more.
Common problems
We also have information on challenges in the early days:
- Breast engorgement and oversupply
- Is my baby feeding well?
- Sore nipples, inflamed ducts, mastitis, thrush
- Tongue tie
- Night feeds
What are other breastfeeding challenges?
When the mother or birthing parent and baby are separated after birth, for example after a caesarean birth or if the baby is premature or goes into special care, there might be a delay in skin-to-skin contact. Ask for support with skin-to-skin contact as soon as possible.
Using a dummy or pacifier before breastfeeding is going well might affect milk production. It is recommended to wait until breastfeeding is well established.
As they get older, babies can sometimes go through a short period of time refusing breastfeeds.
Social challenges
Breastfeeding rates in the UK are very low, and 8 in 10 women and breastfeeding parents stop before they plan to (Unicef, no date).
This is believed to be because breastfeeding is not simply a decision made by the mother or birthing parent. It is part of a complex social system (Trickey, 2018).
Many parents who wanted to breastfeed and stopped before they planned to (Thomson et al, 2022):
- had lower confidence because of stories that it could be hard
- had babies who had an unplanned formula top-up while in hospital
- received conflicting information from healthcare professionals
- were not supported by family and friends
- didn’t seek support with feeding
How can fathers and co-parents support breastfeeding?
Support from fathers and co-parents is known to make a real difference to successful breastfeeding (Erdoğan et al, 2025; Hamnøy et al, 2025).
Here are 10 tips to support a mother or parent to breastfeed:
- Listen and talk honestly about how you each feel about finding your way with your new baby.
- Be positive and encourage progress. As with learning any new skill, reassurance and praise boost confidence.
- Share the caring. Bathing, nappies, playing, massage, talking, singing, and carrying are all great ways of engaging and bonding with the baby.
- Breastfeeding takes a lot of time, so taking care of the household chores can help.
- Help them to relax by giving them a massage if they would like that.
- Provide access to healthy food by making meals and getting them drinks while they’re breastfeeding.
- Encourage access to specialist support if they're struggling. You can both talk to one of our Breastfeeding Counsellors on 0300 330 0700.
- Some parents decide to share care by bottle feeding expressed milk once breastfeeding is established. Bear in mind this doesn’t remove the load from the person who must express.
- Some partners want to help with night feeds, but this doesn’t always work if the mother is woken by the baby anyway.
- Accept your partner’s decision on when to continue or stop breastfeeding.
You may find our article on breastfeeding and sex useful.
Can I breastfeed in public?
You have the right to breastfeed in a public place, such as a café, restaurant, shop, park or public transport. Some places provide quiet spaces for breastfeeding, for parents who wish to use them (NHS, 2023c).
It is illegal to ask someone to stop breastfeeding or go elsewhere to breastfeed. No-one should ever be made to feel like they have to breastfeed in the toilets (NHS, 2023c).
Further information
We also have information on other ways of feeding babies:
As the baby gets older you can also read our articles on:
Breastfeeding Network (no date) How to breastfeed. https://www.breastfeedingnetwork.org.uk/breastfeeding-information/getti… [7 Jul 25]
Erdoğan E, Özerdoğan N. (2025) Evaluation of the effect of the father's support on the mother's breastfeeding motivation. J Eval Clin Pract. 31:e14156. https://doi.org/10.1111/jep.14156
Hamnøy, I.L., Kjelsvik, M., Baerug, A.B. et al. (2025) Fatherhood and breastfeeding: a qualitative exploration of counselling experiences. Int Breastfeed J 20, 36. https://doi.org/10.1186/s13006-025-00730-8
Kim SY, Yi DY. (2020) Components of human breast milk: from macronutrient to microbiome and microRNA. Clin Exp Pediatr. Aug;63(8):301-309. https://doi.org/10.3345/cep.2020.00059
La Leche League GB. (2021) How milk production works. https://laleche.org.uk/how-milk-production-works/ [7 Jul 25]
NHS (2022) Breastfeeding your premature baby. https://www.nhs.uk/baby/breastfeeding-and-bottle-feeding/breastfeeding/… [27 Jun 25]
NHS (2023a) Your breastfeeding questions answered. https://www.nhs.uk/baby/breastfeeding-and-bottle-feeding/breastfeeding/… [27 Jun 25]
NHS (2023b) Breastfeeding: the first few days. https://www.nhs.uk/baby/breastfeeding-and-bottle-feeding/breastfeeding/… [27 Jun 25]
NHS (2023c) Breastfeeding in public. https://www.nhs.uk/baby/breastfeeding-and-bottle-feeding/breastfeeding/… [27 Jun 25]
NHS (2023d) Breast reduction (female). https://www.nhs.uk/tests-and-treatments/cosmetic-procedures/cosmetic-su… [21 Jul 25]
NHS Start for Life (no date) Breastfeeding with breast implants. https://www.nhs.uk/start-for-life/baby/feeding-your-baby/breastfeeding/… [21 Jul 25]
Riskin, A., Almog, M., Peri, R. et al. (2012) Changes in immunomodulatory constituents of human milk in response to active infection in the nursing infant. Pediatr Res 71, 220–225. https://doi.org/10.1038/pr.2011.34
Thomson G, Ingram J, Clarke J, Johnson D, Jolly K (2022) Who Gets to Breastfeed? A Narrative Ecological Analysis of Women's Infant Feeding Experiences in the UK. Front. Sociol. 7:904773. https://doi.org/10.3389/fsoc.2022.904773
Trickey H. (2018). Theorising Breastfeeding Peer Support as an Intervention in a Complex Ecological System: Lessons for Implementation and Evaluation in a Welsh Context. PhD thesis. https://core.ac.uk/download/pdf/200757682.pdf [30 Jul 25]
Unicef (no date) Breastfeeding in the UK. https://www.unicef.org.uk/babyfriendly/about/breastfeeding-in-the-uk/ [30 Jul 25]
WHO (no date) Breastfeeding: Recommendations. https://www.who.int/health-topics/breastfeeding [28 Jul 25]