Babies often lose some of their birth weight in the first three or four days of life, and that’s normal. This is usually just body fluids (NICE, 2017). After this they should gain weight steadily and return to their birth weight by three weeks of life (NICE, 2017; NHS, 2022).
If babies lose more than 10% of their birth weight in the first few days, it’s important to talk to a midwife, health visitor or GP about it (NICE, 2017).
How do I know my baby is getting enough milk?
All babies are different. But if a baby is feeding well – no matter how they are fed – they will have (Unicef, no date):
- Frequent wet, heavy nappies (around six a day from day 5 onwards)
- Two soft poos or more a day
- Weight gain and growth
- A normal skin colour
They will also be (NHS, 2022; Unicef, no date):
- Calm and relaxed
- Content after feeds
- Healthy and alert
- Waking for feeds
What are signs they aren’t feeding well?
A baby who isn’t meeting these points may not be feeding well. They may also show signs of:
- ineffective suckling while breastfeeding, or breastfeeding is painful
- ineffective bottle feeding
- being unsettled after feeds
- being very sleepy and difficult to wake
Our feeding pages have more information on breastfeeding, bottle feeding and combination feeding.
My baby is not gaining weight, what do I do?
If your baby isn’t meeting the points above, talk to the health visitor or GP. You can also speak to a breastfeeding counsellor or lactation consultant to take a look at how feeding is going.
Our NCT Infant Feeding Line provides infant feeding support from 8am to midnight, every day of the year, including bank holidays. Call 0300 330 0700 (option 1).
How much milk do I need to give my baby?
As with adults, babies need different amounts of food, so get to know your baby.
Babies may also need a different amount each day, and will take this in different sized portions. So they won’t necessarily feed for say, 25 minutes each time, or have 4 oz of milk at every feed.
Breastfed babies
It can be hard to ‘measure’ how much milk your baby is getting when breastfeeding. As well as meeting the points above, you can feel reassured if (Unicef, 2016):
- The baby is having at least 8-12 feeds (or more) in 24 hours
- They are feeding for between 5 and 40 minutes at each feed
- Breastfeeding is comfortable
- After 3-4 days old, frequent swallowing should be heard during each feed
- From the fourth day, they should do at least two soft, yellow poos the size of a £2 coin every day for the first few weeks (NHS, 2022)
It might be surprising how much breastfed babies feed. If you are concerned about your baby feeding too much or too little, call our Infant Feeding Line on 0300 330 0700.
Formula-fed babies
As with breastfeeding, make sure your baby is meeting the points above. Also (NHS, 2024):
- Feed your baby 8-12 times a day
- Feed your baby when they seem hungry
- Don’t force them to finish the bottle if they don’t seem to want it
- If the baby is under two weeks old and has not done a poo for 2-3 days, talk to the midwife, health visitor or GP
Mixed feeding
When a baby isn’t exclusively breastfed or exclusively formula fed, it can be hard to tell exactly how much they are getting. The best way to tell they’re getting enough is by regular wet and dirty nappies (NHS, 2022).
They should be having 8 to 12 feeds a day by breast or bottle. Follow your baby's feeding cues to recognise when they’re hungry.
Practicing responsive feeding, giving them milk when they show feeding cues, can help make sure they are getting the milk when they need.
After a feed from the breast or bottle, the baby should come off the breast or move away from the bottle. If they’re then happy and relaxed, this suggests they’ve had enough and are content (NHS, 2022). Talk to a health visitor or GP if you’re worried. You can also call our Infant Feeding Line on 0300 330 0700.
What is responsive feeding?
Responsive feeding works well for both bottle and breastfed babies. Let your baby guide you as to how often they want to feed (Unicef, 2022).
When bottle feeding, let the baby take a little bit of milk. When you see a pause from sucking then stop and let them take more when they’re ready. This mimics breastfeeding and prevents overfeeding (NHS, no date). This kind of paced feeding allows them to stop when they’re content.
Why do babies feed so often?
Babies have small tummies, and tend to feed little and often. This is the same for all babies, whether they are fed at the breast or chest, by bottle or a mixture of both (NHS, no date; Unicef, 2022).
Feeding is more than just nutrition – it means a time of closeness and comfort with their caregiver (Unicef, 2022).
How do I know if I’m giving my baby too much milk?
Breastfeeding
It’s not possible to overfeed a breastfed baby (NICE, 2021; Unicef, 2022). Babies may want to breastfeed a lot, but it doesn’t necessarily mean they are not getting enough milk or too much. It’s very rare for a mother or birthing parent not to make enough milk for the baby (Unicef, 2022).
If a baby is breastfed when they show feeding cues, and at least 8-12 times in 24 hours, they won’t be getting too much.
See our pages on how to breastfeed for signs that breastfeeding is going well.
Bottle feeding
Don’t encourage your baby to finish a bottle if they don’t want to, unless a midwife or health visitor has said that there are concerns about lack of weight gain. Babies know how much milk they need and making them take more can be stressful for them (NHS, no date; Unicef, 2019).
Mixed feeding
When mixed feeding, it can be hard to judge how much the baby is getting.
As with exclusive formula feeding, don’t make them finish the bottle at a feed if they don’t seem to want it all. But as with exclusive breastfeeding, you don’t need to shorten breastfeeds as they can’t be overfed on the breast.
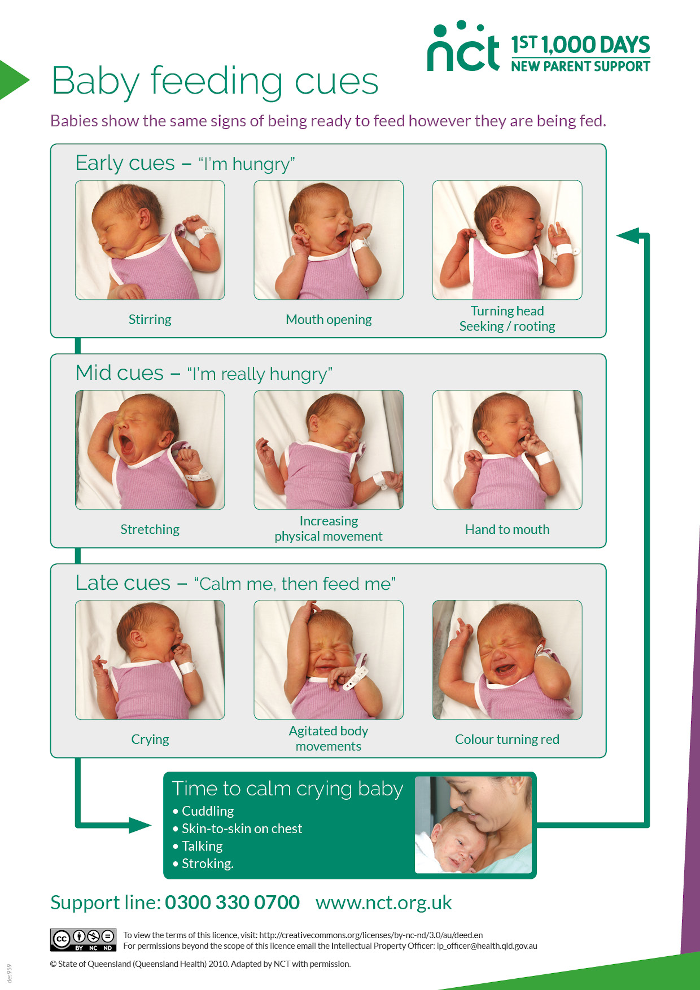
Feeding cues
The baby will show you it is hungry by (NHS, no date):
- Trying to find something to suck
- Looking around
- ‘Rooting around’ looking for the nipple or bottle teat with an open mouth
- Getting restless and wriggly
- Opening and closing their mouth
How can the non-feeding parent enjoy closeness with the baby?
A baby isn't just getting food and fluid from a feed. They’re also getting love and security. Even if the baby is being exclusively breastfed, the non-feeding parent can give the baby the same feeling of closeness and warmth by:
- Cuddling
- Rocking
- Holding the baby
- Enjoying quiet time together
Karen Hall (2023) Why Mixed Feeding Matters (book) Pinter and Martin: London pp88-89 [Accessed 3 June 2025]
NHS Better Health Start for Life (no date) Feeding on demand https://www.nhs.uk/start-for-life/baby/feeding-your-baby/bottle-feeding/bottle-feeding-your-baby/feeding-on-demand/ [Accessed 3 June 2025]
NHS (2022) Breastfeeding: Is my baby getting enough milk? https://www.nhs.uk/baby/breastfeeding-and-bottle-feeding/breastfeeding-problems/enough-milk/ [Accessed 3 June 2025]
NHS (2024) Bottle Feeding Advice https://www.nhs.uk/baby/breastfeeding-and-bottle-feeding/bottle-feeding/advice/ [Accessed 3 June 2025]
NICE guideline Reference number: NG75 Published: 27 September 2017 https://www.nice.org.uk/guidance/ng75 [Accessed 3 June 2025]
NICE guideline Reference number: NG194 Published: 20 April 2021 https://www.nice.org.uk/guidance/ng194/chapter/Recommendations#planning-and-supporting-babies-feeding [Accessed 3 June 2025]
Unicef The Baby Friendly Initiative Bottle Feeding Assessment Tool (no date) https://www.unicef.org.uk/babyfriendly/baby-friendly-resources/bottle-f… [Accessed 3 June 2025]
Unicef The Baby Friendly Initiative Mothers Breastfeeding Checklist (no date) https://www.unicef.org.uk/babyfriendly/wp-content/uploads/sites/2/2016/… [Accessed 3 June 2025]
Unicef Responsive bottle feeding (no date) https://www.unicef.org.uk/babyfriendly/wp-content/uploads/sites/2/2019/… [Accessed 3 June 2025]
Unicef/NHS Off to the best start (no date) https://www.unicef.org.uk/babyfriendly/wp-content/uploads/sites/2/2022/… [Accessed 3 June 2025]







