Antenatal screening and diagnostic tests can detect pregnancy complications and foetal anomalies. Find out here what you and your baby may be tested for.
During pregnancy you will be offered antenatal screening tests which check and assess the well being of you and baby. They can also identify genetic conditions such as Down's syndrome, Edwards' syndrome and Patau's syndrome. All tests are optional, it is your choice as to which tests you have or don't have. It is important to understand the conditions you are potentially testing for in order to be able to make informed decisions as to which tests, if any, you wish to have.
Pregnancy and foetal screening tests may include blood tests (screening for conditions such as sickle cell anaemia) and scans (such as nuchal translucency scan which looks at the likelihood of baby having a genetic condition).
A screening test can only give you information about how likely it is that your baby may be affected by a condition. If the likelihood is high, you will be offered a diagnostic test, which can give you a definite answer.
Available foetal and pregnancy screening tests
There are a number of foetal screening tests that are offered as part of your antenatal care. this article covers:
- the anomaly scan
- screening for spina bifida
- screening for sickle cell and thalasaemia
- screening for Down's syndrome
- chorionic villus sampling (CVS)
- amniocentesis
- cystic fibrosis
- non-invasive prenatal testing
Before you make any decisions, it is important that you (and your partner) think about the implications of going ahead with any pregnancy screening tests.
The anomaly scan
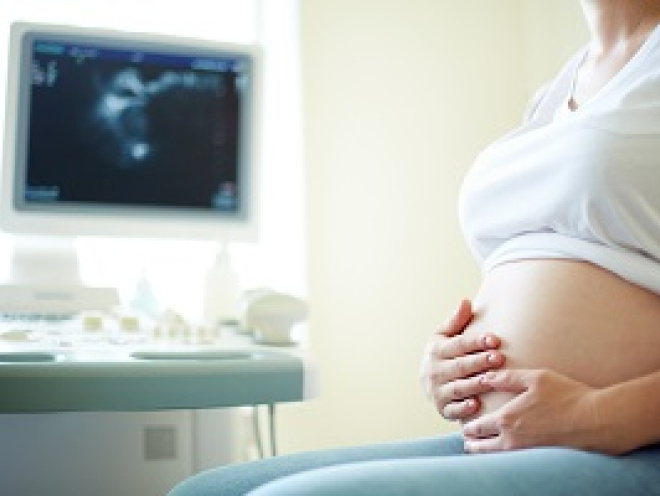
All pregnant women are offered the opportunity to have an anomaly scan between 18 and 21 weeks. The anomaly scan is a detailed pregnancy scan that checks the structure and organs of your baby, including the brain, heart and lungs.
"The anomaly scan is not 100% guaranteed to pick up a specific problem like a genetic abnormality. You can ask at your hospital about detection rates of these scans."
Although you do not have to wait for ‘results’, sometimes you may need to have the scan repeated, either:
- because the picture is not clear due to the way the baby is lying or moving or
- because the sonographer would like to refer you to someone with specialist expertise or with better equipment.
There is no evidence to suggest that the ultrasound used in the antenatal scan harms your baby. Pregnancy scans do not use the ionising radiation used in other medical diagnostic procedures, which may carry a small risk to the baby.
Spina bifida
The anomaly scan will include a check of your baby’s spine to try to rule out major spina bifida. Spina bifida is also known as a neural tube defect (NTD) which can occur very early on in pregnancy. The disabilities caused by spina bifida range from back pain, weakness in the lower limbs and bowel/bladder problems, to paralysis of the lower half of the body and incontinence.
Taking extra folic acid before you become pregnant and in the first three months as part of a healthy pregnancy diet, could help reduce the likelihood of neural tube defects, such as spina bifida.
Screening for Down’s syndrome
Screening for Down’s syndrome and other genetic conditions is offered to all pregnant women. There are are a range of Down’s syndrome screening tests, and if the screening shows a high likilihood, then a diagnostic test will be offered.
Screening for sickle cell and thalassaemia
All pregnant women will be asked questions about their family origins to see if they should be offered a blood test to screen for sickle cell disorder and thalassaemia.
Sickle cell disorder is a genetic abnormality of the blood that affects people from Africa, the Caribbean, the Eastern Mediterranean, Middle East and Asia. The disorder affects the quality of red blood cells. If both the mother and father are found to be carriers of sickle cell gene, they will be offered an amniocentesis or chorionic villus sampling (CVS) to see if their baby has the disease.
Thalassaemia is a genetic abnormality of the blood affecting people from Africa, Asia, the Middle East and the Mediterranean. Symptoms include anaemia and attacks of severe pain. If both the mother and father are found to be carriers of the thalassaemia gene, they will be offered an amniocentesis or CVS to see if their baby has the disease.
Cystic fibrosis
Cystic fibrosis affects the internal organs, especially the lungs, pancreas and digestive system, by clogging them with thick sticky mucus. Cystic fibrosis is a potentially life-threatening, genetically inherited disease.
If a couple are both carriers of the cystic fibrosis gene, the baby has a one in four chance of having cystic fibrosis. There is no routine UK-wide antenatal screening for cystic fibrosis. However, for those who know they are at risk, an antenatal test is available – a chorionic biopsy carried out at around nine weeks after conception or amniocentesis at about 15 weeks – to identify if the unborn baby has cystic fibrosis.
Babies are screened postnally for cystic fibrosis at around six days by the ‘blood spot’ or Newborn Screening Test.
What is chorionic villus sampling (CVS)?
Chorionic villus sampling (CVS) is a diagnostic test that you’ll be offered if you have a higher chance of carrying a baby with a chromosomal or genetic condition. CVS involves the removal and testing a small sample of cells from the placenta.
The process involves inserting a needle through your tummy (transabdominal CVS) or a tube inserted through the cervix (transcervical CVS). It is usually uncomfortable rather than painful, and can lead to period-like cramps afterwards (RCOG, 2010; NHS, 2018, ARC, 2019). You should take it easy for the next 48 hours or so after having the test (ARC, 2019).
Doctors are able to perform CVS earlier in the pregnancy than amniocentesis, at between 11 and 14 weeks. It will not be performed before 10 weeks (Payne, 2016). Although it can be performed earlier, CVS carries a very slightly higher risk of miscarriage than an amniocentesis performed between weeks 15 to 18 of pregnancy (Payne, 2016).
Unfortunately, about one in 100 mums who have a CVS will miscarry (ARC, 2019).
What is amniocentesis?
Like CVS, amniocentesis is a diagnostic test that you’ll be offered if you have a higher chance of carrying a baby with a chromosomal or genetic condition. It is carried out between 15 and 18 weeks. This is the safest time to have the test as there is more risk of miscarriage earlier in pregnancy (Payne, 2016).
During the test, a needle is inserted through your abdominal wall and a small amount of amniotic fluid that surrounds the baby will be taken and tested (Payne, 2016). Amniocentesis when performed from 15 to 18 weeks carries a slight risk of miscarriage, of about 0.5%-1%.
You may feel worried if you need to have this but try to remember that it’s not an uncommon test. About 5% of mums-to-be are offered CVS or amniocentesis (Payne, 2016).
Non-invasive prenatal testing (NIPT)
From 2018, the NHS started to roll out a non-invasive prenatal test (NIPT) screening test for Down’s, Edwards’ and Patau’s syndromes (Gov.UK, 2019).
The test analyses a sample of blood taken from mum and can be done from 10 weeks of pregnancy as your blood will contain DNA from the placenta. This DNA can be analysed to see whether there is a higher chance of your baby having Down's syndrome, Edwards' syndrome or Patau’s syndrome.
Women can get false positive and false negative results so an invasive test will still be required to confirm whether or not baby has a genetic condition. There are currently private providers who offer NIPT (you may have heard of the Harmony Test, for example).
Last updated: May 2019
Further information
Our support line offers practical and emotional support in all areas of pregnancy, birth and early parenthood: 0300 330 0700. We also offer antenatal courses which are a great way to find out more about birth, labour and life with a new baby.
The NHS gives information on its website about the Sickle Cell and Thalassaemia Screening Programme.
You could also contact www.shinecharity.org.uk and www.downs-syndrome.org.uk and https://positiveaboutdownsyndrome.co.uk/ for more information and support.
The Sickle Cell Society offers information, counselling and caring for those with Sickle Cell disorders and their families.
The Spina Bifida Association is Europe’s largest organisation dedicated to supporting individuals and families as they face the challenges arising from spina bifida and hydrocephalus. The website includes information on folic acid and the prevention of spina bifida.
Go Folic! is a campaign led by the Association for Spina Bifida and Hydrocephalus and Scottish Spina Bifida Association, calling on women to take folic acid during and prior to pregnancy.
Mencap supports the 1.4 million people with a learning disability in the UK and their families and carers. Mencap fights to change laws and improve services and access to education, employment and leisure facilities, supporting thousands of people with a learning disability to live their lives the way they want.
The Cystic Fibrosis Trust offers information about the causes, symptoms and treatments of CF along with details about day to day living with Cystic Fibrosis. Helpline: 0300 373 1000.
RCOG (Royal College of Obstetricians and Gynaecologists) offers a guidance sheet about amniocentesis and chorionic villus sampling.
NHS gives full information on the checks and tests offered in pregnancy.
Healthtalkonline offers shared experiences, videos and stories from 37 women and 8 couples from the UK. Topics include making decisions about screening, including those that have and have not ended the pregnancy.
ARC (2019) Tests explained. Available at: https://www.arc-uk.org/tests-explained [Accessed 20th May 2019].
NHS. (2018) Screening for Down’s Edwards and Pataus’ syndrome Avaliable at: (https://www.nhs.uk/conditions/pregnancy-and-baby/screening-amniocentesi… [Accessed 26/05/19].
Payne J. (2016) Amniocentesis. Available at: https://patient.info/doctor/amniocentesis-pro [Accessed 20th May 2019].
RCOG. (2010) Amniocentesis and chronic villus sampling. Available at: https://www.rcog.org.uk/en/guidelines-research-services/guidelines/gtg8/ [Accessed 20th May 2019].