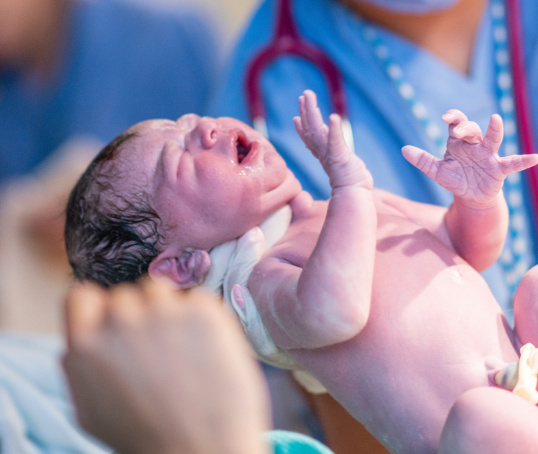
You can find out more about how labour progresses on our NCT Antenatal course. You can also read about the first stage and third stage of labour.
Latent second phase – ‘rest and be thankful’
The passive or latent phase is commonly known as ‘rest and be thankful’.
The contractions that were pulling the cervix open pause. The woman or person in labour can rest, have a drink, and change position.
This might be quite short, and the labouring woman or person might not notice it. Or it could last for more than an hour. If there is an epidural, then a longer pause is expected (NICE, 2023).
Active phase – birthing the baby
This is the active, birthing part, when the baby is pushed out from the uterus through the vagina. This might last minutes or hours (NICE, 2023).
- At some point, the woman or birthing person usually experiences a strong and involuntary urge to push (NICE, 2023).
- The muscles which were pulled up behind the baby as the cervix was pulled open are now contracting to push out the baby or babies from the womb.
Women and birthing people sometimes say the start of the active second stage is a relief:
- For some, contractions feel easier to cope with and they let go and let the body work (Häggsgård et al, 2021).
- There is a new sense of alertness and energy, and the contractions feel different from the first stage. This is the hormones working to support the birth of the baby.
- The baby also receives hormones to help them cope with this part of labour.
- Birthing contractions are longer than the labouring ones, but the gaps between them are also longer.
Sometimes the waters break before labour starts, but most commonly they break during the second stage. Sometimes they don’t break at all. This is not a problem, and the midwife will break them after the baby is born.
How is the baby born?
As the baby moves down, the shape of the pelvis and pelvic floor means the baby’s body turns, taking the easiest path. The baby’s soft head also moulds to fit. It will go back to a normal shape in the hours after birth.
As the baby’s head (or bottom if the baby is breech) becomes visible, the perineum (the area between the vagina and anus) needs to stretch slowly to reduce the chance of tearing. There might be a sense of burning or stinging (Häggsgård et al, 2021).
The midwife might encourage the woman or birthing person to take short breaths or pant (NHS, 2023). Read more about common concerns about giving birth.
The baby’s head is born with one contraction, then there is a pause before the rest of the body is born with the next contraction.
Very occasionally the baby’s shoulder gets temporarily caught in the pelvis (shoulder dystocia).
How long does the active phase last?
If this is the first baby, birth is expected within three hours (NICE, 2023):
- if the baby is not born after an hour, the midwife will assess the situation
- after two hours, the midwife will consult with a doctor
When the mother or birthing person has had a baby before, birth is expected within two hours (NICE, 2023):
- if the baby is not born after 30 minutes, the midwife will assess the situation
- after an hour, the midwife will consult with a doctor
What happens if labour is not progressing?
If no contractions are felt, or labour isn’t progressing, the midwife will offer support. They might suggest (NICE, 2023):
- changing position
- going for a wee to empty the bladder and make more room for the baby
- breaking the waters if not already broken
The pregnant woman or person may be offered pain relief (NICE, 2023).
The doctor’s review might suggest (NICE, 2023):
- an oxytocin drip to strengthen contractions
- additional pain relief
- birth by forceps or ventouse
- birth by caesarean
What does pushing feel like?
Typically, it is impossible not to push when the body has the urge to. There is a sense of fullness in the pelvis, and pressure downwards. If there is no epidural, there may be an awareness of the baby moving down (Häggsgård, 2021; Reed, no date a).
It’s useful to know that expulsive contractions are beyond the labouring woman or person’s control, and it’s not necessary for them to try to make their body do this. Unconscious women are known to give birth (Hofmeyr & Singata-Madliki, 2020).
While some women and birthing people appreciate the midwife telling them how and when to push, others want to be guided by their own body and retain control (Häggsgård et al, 2021).
For some the strong sensations give positive feelings of power and wonder, while for others it can feel overwhelming and frightening. This explains why feeling supported and listened to is vital (Häggsgård et al, 2021).
If a woman or birthing person is not feeling an urge to push, then it may be that they are still in the latent phase. In that case, moving around, relaxing, and hydrating may all help.
How to push?
The National Institute of Health and Care Excellence (NICE) recommends spontaneous pushing where labour is progressing well. That is, for the labouring woman or person to follow their own body without anyone telling them what to do (NICE, 2023).
Pushing directed by the midwife, and while exhaling, might be recommended to shorten the second stage in some situations. Pushing with held breath is tiring and not recommended (Hofmeyr & Singata-Madliki, 2020; NICE, 2023).
Women and birthing people use a wide range of strategies such as (Häggsgård et al, 2021):
- either making noise, or going silent
- focused breathing
- moving
- concentrating on what’s happening inside the body
Some women and birthing parents find it helpful to use a mirror or touch the baby’s head and body as it emerges. This helps them to feel connected to the baby and overcome exhaustion. It helps them control their pushing efforts (Häggsgård et al, 2021).
What positions are best for labour?
TV shows and movies often depict the pregnant woman or person lying on their back on a hospital bed. However, this can lead to pressure on major blood vessels and reduce blood flow to the baby, so is not recommended (Hofmeyr & Singata-Madliki, 2020; NICE, 2023).
Upright or side-lying positions, where the sacrum (the back of the pelvis) can be flexible, lead to a shorter second stage (Berta et al, 2019).
Women or birthing parents should be supported to find a position or positions that work for them. This could be (Hofmeyr & Singata-Madliki, 2020; NICE, 2023):
- in water
- using a birthing ball
- squatting
- standing
- kneeling
- lying on one side
How do we know everything is ok?
At least one midwife will be in the room during the active second stage of labour. They continue to monitor the mother or birthing person and baby as before, but more frequently (NICE, 2023).
The baby’s heart rate will be checked at least every 5 minutes. A vaginal examination will be offered hourly (NICE, 2023).
The midwife should be someone the woman or birthing parent can trust. They should provide information and guidance, so the woman or birthing person can make an informed decision (Häggsgård et al, 2021; NICE, 2023).
If there is a lack of confidence in the healthcare professional at any point in labour, it is encouraged to ask for a second opinion or a different caregiver (The Patients Association, no date).
How can a birth partner, father or co-parent support?
Having a trusted co-parent or birth partner provides security (Häggsgård et al, 2021). This support can include (Yuksel et al, 2017):
- encouraging deep breathing between contractions
- advocating for the pregnant woman or person
Read our article on birth partners and doulas.
Common concerns about birthing the baby
If you’re a pregnant woman or person and you’re worried about what will happen in labour, you can talk to your midwife for guidance and reassurance. Here we address some common concerns.
What is an anterior lip?
Some labouring women and people feel an urge to push before their cervix has fully dilated. They may be told there is an ‘anterior lip’. This is normal.
- The cervix opens in an oval shape, with the front part the last to move over the baby’s head (or bottom).
- It is only spotted if a vaginal examination is done at this point (Reed, no date a)
- The contractions will push the baby through as the cervix opens.
- Sometimes, the midwife moves the remaining part of cervix out of the way.
- There is no evidence to suggest that pushing with an anterior lip is harmful to mother or baby (Hofmeyr & Singata-Madliki, 2020; Reed, no date a).
Tearing and episiotomy
The perineum is the area between the vagina and anus. Many women and birthing people are anxious about the chance of this tearing or being cut.
- The midwife will encourage short breaths or pants, so that the perineum can stretch slowly. This may reduce the risk of tearing (Ibrahim et al, 2017).
- Using a mirror or touching the baby’s head can help control the pushing efforts.
- No decision to cut the perineum will be made without the woman or birthing parent’s consent (NHS, 2023).
Read our article, which explains tearing and episiotomy in more detail.
What is shoulder dystocia?
Shoulder dystocia (diss-TOH-shee-uh) is when the baby’s shoulder is temporarily caught in the pelvis during the birth. It happens in between 6 and 7 in 1000 births (RCOG, 2012). If not quickly resolved, it can lead to health problems for the baby. All midwives train regularly in dealing with shoulder dystocia.
Induction is sometimes offered if the baby is estimated to be over 4.5kg, because there is a concern about shoulder dystocia (RCOG, 2012).
However (RCOG, 2012):
- it is hard to measure the size of the baby
- most babies over 4.5kg do not experience shoulder dystocia
- almost half of the babies who do experience shoulder dystocia are under 4.0kg
So the Royal College of Obstetricians and Gynaecologists (RCOG) say this shouldn’t be used as a reason for induction (RCOG, 2012).
What if the umbilical cord is around the baby’s neck?
One in three babies has their umbilical cord wound around their neck at birth. This is called a nuchal cord (Reed, no date b).
The cord has evolved to be very tough, so this is almost never a problem to the baby’s supply of oxygen (Reed, no date b).
When babies are born with the cord around their neck it may be slipped over their head as they are born, or they somersault out and it is removed later. It is unusual for it to cause complications (Reed, no date b).
What happens after the baby is born?
As you welcome your baby, the body prepares for the third stage of labour, when the placenta is born. Read more about the birth of the placenta in our article.
There’s also skin-to-skin with your baby and much more, which we’ve explained in another article.
BJOG: An International Journal of Obstetrics & Gynaecology, 118: 662-670. https://doi.org/10.1111/j.1471-0528.2011.02910.x
Berta M, Lindgren H, Christensson K, Mekonnen S, Adefris M. (2019) Effect of maternal birth positions on duration of second stage of labor: systematic review and meta-analysis. BMC Pregnancy Childbirth. 19(1):466. https://doi.org/10.1186/s12884-019-2620-0
Häggsgård C, Nilsson C, Teleman P, Rubertsson C, Edqvist M. (2021) Women’s experiences of the second stage of labour. Women and Birth. 35(5):e464-e470. https://doi.org/10.1016/j.wombi.2021.11.005
Hofmeyr G, Singata-Madliki M. (2020) The Second Stage of Labour. Best Practice Research Clinical Obstetrics Gynaecology. 67:53-64. https://doi.org/10.1016/j.bpobgyn.2020.03.012
Ibrahim H, Ghattas V, Abd H, Kandeel E. (2017) Effect of breathing technique (blowing) on the integrity of perineum and duration of the second stage of labor among primiparous women. World Journal of Nursing Sciences. 3(3). https://www.researchgate.net/publication/348610324_Effect_of_Breathing_… [27 Jan 25]
NHS (2023) The stages of labour and birth. https://www.nhs.uk/pregnancy/labour-and-birth/what-happens/the-stages-o… [5 Feb 25]
NICE. (2023) Intrapartum care [NG235] https://www.nice.org.uk/guidance/ng235 [30 Jan 25]
Prins, M., Boxem, J., Lucas, C. and Hutton, E. (2011), Effect of spontaneous pushing versus Valsalva pushing in the second stage of labour on mother and fetus: a systematic review of randomised trials.
RCOG (2012) Shoulder dystocia. (Green-top Guideline No. 42). https://www.rcog.org.uk/guidance/browse-all-guidance/green-top-guidelines/shoulder-dystocia-green-top-guideline-no-42/ [26 Nov 24]
Reed R (no date a) The Anterior Cervical Lip: how to ruin a perfectly good birth. https://www.rachelreed.website/blog/the-anterior-cervical-lip-how-to-ru… [27 Jan 25]
Reed R (no date b) Nuchal cords: the perfect scapegoat. https://www.rachelreed.website/blog/nuchalcords [30 Jan 25]
The Patients Association (No date) Getting a second opinion. https://www.patients-association.org.uk/getting-a-second-opinion [14 Nov 24]